Understanding Emphysema: Insights and Implications

Intro
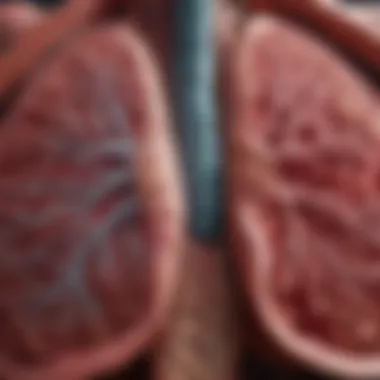
Emphysema is not just a medical term; it's a complex condition that affects millions around the globe. Often seen as just another respiratory issue, it carries with it a heavy burden—both for the individuals grappling with its realities and for the healthcare systems that strive to manage its implications. In essence, emphysema causes the gradual destruction of the alveoli, small air sacs in the lungs that are crucial for oxygen exchange. This destruction leads to a host of respiratory difficulties that go beyond mere breathlessness.
Understanding the nuances of emphysema involves looking at its underlying mechanics, the various risk factors that contribute to its development, and the diagnostic methods that can detect it in its early stages. Furthermore, the condition doesn’t exist in a vacuum. Its social implications affect patients' quality of life, emotional well-being, and social interactions, while there are economic costs that society bears. As research continues to evolve, it becomes vital to shed light on treatment options and preventive measures that can potentially alter the course of this disease.
Through a thorough exploration of these elements, the intent of this article is clear: to provide a clearer picture of emphysema, emphasizing its complexities, its challenges, and the pathways toward better health outcomes.
Intro to Emphysema
Emphysema is more than just a medical term; it represents a profound challenge faced by a segment of our population. This introductory section aims to unpack the intricacies of this respiratory affliction. By shedding light on emphysema, we explore its vital connections with health, lifestyle, and socio-economic factors.
Understanding emphysema holds considerable significance, primarily because its effects resonate through families, communities, and the healthcare system at large. The condition is linked to chronic respiratory disorders, significantly impacting the quality of life for many individuals. The insights provided in this section set the stage for deeper exploration into emphysema’s mechanisms, risk factors, and the interplay it has with broader health issues.
Definition and Overview
At its core, emphysema is a progressive lung disease that primarily affects the alveoli—the tiny air sacs within the lungs. When these alveoli become damaged, they lose their elasticity, making it increasingly difficult for the lungs to function properly. This leads to increasing levels of trapped air, which not only makes breathing laborious but also results in decreased oxygen intake.
A clear, simple understanding would note that emphysema doesn’t just appear overnight. It develops gradually, often many years after initial lung damage, usually associated with smoking or long-term exposure to irritants. For clarity:
- Alveoli Damage: The walls between many of the alveoli are destroyed, leading to larger air spaces instead of many small ones.
- Air Trapping: The damaged alveoli cannot fully expel air, contributing to overinflation of the lungs.
- Symptoms: Common issues include shortness of breath, coughing, and wheezing.
The connection of emphysema to broader health issues is crucial. For instance, it commonly coexists with chronic bronchitis, another form of chronic obstructive pulmonary disease (COPD). Understanding the definition and the biological underpinnings of this disease is the first glimpse into the larger puzzle of respiratory health.
Historical Context
Emphysema has not always been recognized or understood as a distinct condition. Throughout history, the perception of lung disorders has evolved significantly. In the early 20th century, emphysema was often lumped together with other respiratory issues, and the medical community only began separating it from related ailments as research advanced.
A significant turning point came with the industrial boom and the alarming rise of workers’ exposure to harmful fumes. In the 1950s, research started to identify emphysema specifically linked to smoking. For those interested in the evolution:
- Early Recognition: Before the mid-1900s, emphysema was not clearly distinguished from general lung disease.
- Research Focus: Increased research led to a better understanding of the disease, and public health campaigns emerged to inform about the dangers of smoking.
- Treatment Advances: The late 20th century emphasized better management options and pulmonary rehabilitation, which have improved the quality of care.
"Understanding the historical context allows for a more profound appreciation of how far we've come in managing and treating emphysema, which was once seen merely as a consequence of aging or environment."
Emphysema not only illustrates the impact of lifestyle choices on health but also highlights the importance of ongoing research and public health initiatives. An informed understanding sets the stage for discussing emphysema's pathophysiology, risk factors, and the serious implications for those affected.
Pathophysiology of Emphysema
Understanding the pathophysiology of emphysema is crucial as it elucidates how the condition alters normal lung function. Recognizing these changes provides insight into patient experiences and guides medical professionals in delivering appropriate care. The complexity of emphysema stretches beyond superficial symptoms and requires a meticulous examination of the underlying mechanisms that drive alveolar destruction and respiratory impairment.
Nature of Alveolar Damage
Emphysema is characterized primarily by the damage to the alveoli, the tiny air sacs in the lungs responsible for gas exchange. This process often begins when harmful particles, like those found in cigarette smoke or pollution, infiltrate the lungs. As these particles accumulate, they provoke an inflammatory response that leads to the breakdown of elastin, a protein that maintains the structural integrity of alveoli.
The damage to these air sacs can be likened to a worn-out sponge: once elastic and capable of expanding and contracting, repeated trauma causes them to lose their resilience. Over time, this leads to larger but fewer alveoli, severely reducing the surface area available for oxygen absorption and carbon dioxide removal. Quite literally, the lungs become less capable of handling the fundamental task of breathing.
Inflammatory Processes
The body's immune response plays a pivotal role in the pathophysiology of emphysema. Upon the inhalation of irritants, immune cells, particularly neutrophils and macrophages, swarm to the site of injury in an effort to mitigate damage. However, the lion's share of these immune cells releases enzymes and reactive oxygen species that inadvertently exacerbate lung injury instead of healing it.
This misguided response is akin to pouring gasoline on a fire; it intensifies the damage instead of quelling it. Chronic inflammation in emphysema disrupts the delicate balance between destructive and protective factors, leaving the lungs in a state of ongoing deterioration. As a consequence, this relentless cycle not only hinders healing but also promotes further alveolar damage.
Impact on Gas Exchange
The final fallout of alveolar damage and chronic inflammation manifests starkly in the efficiency of gas exchange. With fewer functional alveoli, the lungs struggle to oxygenate blood adequately and remove carbon dioxide. Consequently, patients often experience shortness of breath, particularly during exertion.
This inefficiency can lead to severe complications, such as pulmonary hypertension and respiratory failure, fundamentally altering a person's quality of life. The increasingly labored breathing may compel individuals to avoid physical activities, fostering a sedentary lifestyle that compounds existing health issues.
In summary, the interplay of structural damage, inflammation, and impaired gas exchange encapsulates the heart of emphysema's pathophysiology. Understanding these interconnections is essential for developing effective treatment strategies aimed at mitigating this condition's impact.
Risk Factors and Epidemiology
Understanding the risk factors and epidemiology of emphysema is crucial because it helps to identify populations at risk and informs strategies for intervention and management. Recognizing these factors sheds light on how lifestyle choices, genetic predispositions, and various environmental exposures can influence the development and progression of emphysema. This section provides insights into the multifaceted nature of the condition, facilitating a proactive approach in healthcare and public health policy.
Cigarette Smoking
Cigarette smoking stands out as the leading cause of emphysema. The harmful substances in tobacco smoke damage the lung tissues over time, leading to irreversible changes in the alveoli. Smokers, especially those who start at a young age, face the highest risk. In fact, a substantial percentage of emphysema cases occur among long-term smokers. This is not simply a number; it reflects a significant public health issue that requires urgent attention.
Moreover, it’s not only the heavy smokers who are affected; even those who smoke occasionally can still be at risk. Interestingly, there is data showing that even secondhand smoke can increase the chances of developing emphysema.
This emphasizes the importance of education and smoking cessation programs aimed at both smokers and their families.
Genetic Predispositions

While lifestyle factors like smoking play a pivotal role, genetics also significantly influences susceptibility to emphysema. A notable condition that exemplifies this is Alpha-1 Antitrypsin Deficiency (AAT deficiency). Individuals with AAT deficiency have an increased risk because their bodies don't produce enough of the protein that protects the lungs. This genetic aspect underscores the need for genetic screening in individuals with a family history of lung diseases.
It is also worth mentioning that not all smokers will necessarily develop emphysema. Many people who smoke for years have normal lung function. This indicates that genetic factors can be a double-edged sword, affecting how individuals respond to environmental factors.
Environmental Exposures
Apart from smoking and genetics, numerous environmental exposures contribute to the risk of developing emphysema. Occupational hazards such as dust, chemicals, and fumes are significant. For instance, individuals working in industries like construction, mining or agriculture may be exposed to harmful particulates that compromise lung health.
Furthermore, air pollution, a growing global concern, has been linked to increased rates of emphysema. Urban dwellers, who often grapple with poor air quality, can find themselves at heightened risk.
In addition, exposure to indoor pollutants such as biomass smoke from cooking with solid fuels can also play a role, especially in developing countries. It presents a vivid reminder that environmental factors should not be overlooked in discussions about pulmonary health.
In summary, understanding the various risk factors associated with emphysema is imperative for effective prevention and management strategies. Whether it’s focusing on reducing smoking rates, identifying genetic markers, or addressing hazardous environmental conditions, a comprehensive approach can lead to better patient outcomes and public health improvements.
Clinical Manifestations
Understanding the clinical manifestations of emphysema is crucial for both patients and healthcare professionals alike. Recognizing the symptoms and potential complications allows for early intervention and better management of the disease. Additionally, this knowledge can empower individuals to make informed decisions about lifestyle modifications, treatment options, and regular check-ups.
Symptoms Overview
Emphysema presents itself through a variety of symptoms, which can develop gradually. Often, individuals may not even realize how much their breathing has changed until it becomes significantly debilitating. Common symptoms include:
- Shortness of breath: Initially noticeable during exertion, this symptom can progress to occurring even at rest.
- Chronic cough: A persistent cough, often referred to as "smoker's cough," can develop due to lung irritants.
- Wheezing: This whistling sound during breathing could indicate narrowing airways, which is common in emphysema.
- Fatigue: Chronic fatigue often accompanies reduced oxygen levels, leading to a marked decrease in daily functioning.
- Chest tightness: Some patients report feeling pressure in their chest, which can be uncomfortable.
As these symptoms evolve, many find it challenging to engage in daily activities, which adds to the emotional burden often experienced by those living with the disorder. The importance of identifying these symptoms cannot be overstated, as early recognition could lead to timely interventions, enhancing overall quality of life.
Complications Associated with Emphysema
The ramifications of emphysema extend beyond just the respiratory issues. Complications can arise, intertwining with patients’ physical and mental health, creating a complex healthcare scenario. Among these complications, some of the more significant ones include:
- Respiratory infections: Individuals with emphysema are more susceptible to pneumonia and bronchitis due to weakened lungs.
- Lung collapse (pneumothorax): In severe cases, damaged alveoli can lead to air leaking into the chest cavity, resulting in a lung collapse.
- Pulmonary hypertension: This condition arises when blood vessels in the lungs narrow, escalating pressure on the heart, which can lead to right-sided heart failure over time.
- Depression and anxiety: The chronic nature of emphysema, combined with the limitations it imposes, can lead to mental health challenges that often go unnoticed.
"Managing emphysema is not solely about breathing; it is about living and ensuring that patients maintain their quality of life."
Addressing these complications requires a comprehensive approach that evaluates physical health while also considering emotional well-being. Acknowledging the far-reaching effects of this disease fosters a holistic management plan, ultimately improving outcomes and enhancing the overall experience for patients and their families.
Diagnostic Approaches
The realm of emphysema diagnosis is not merely about identifying a respiratory condition; it encapsulates a holistic approach to understanding patient health and designing effective treatment strategies. With emphysema intertwined with varied clinical presentations, the diagnostic strategies provide essential insights that help healthcare professionals tailor interventions. By grasping these approaches, one can not only glean the nuances of the condition but also appreciate the broader implications for patient management.
Pulmonary Function Tests
Pulmonary Function Tests (PFTs) work it like a charm when it comes to diagnosing emphysema. These tests measure lung capacity, airflow, and gas exchange, providing a detailed view of how well the lungs are functioning. Among them, spirometry is often the go-to tool. It assesses FEV1 (forced expiratory volume in one second) and FVC (forced vital capacity). A notable decline in the FEV1/FVC ratio can signal restrictive or obstructive disorders, making it a critical indicator in emphysema evaluation.
- Key Benefits of PFTs:
- Non-invasive nature making it safe for patients
- Ability to track disease progression over time
- Help tailor management plans based on detailed patient data
"Pulmonary function testing offers a window into lung health, revealing truths that the naked eye cannot see."
In evaluating emphysema, the test results must be contextualized with a patient’s history and symptoms. A combination of results not only aids in diagnosing the disease but in distinguishing it from other pulmonary disorders that may have similar symptoms. It’s like having a multi-tool in your diagnostic kit – versatile and essential.
Imaging Techniques
The technical landscape of imaging techniques is another pivotal element in diagnosing emphysema. High-resolution computed tomography (HRCT) has gained considerable acclaim for its ability to showcase lung architecture with remarkable clarity. This imaging technique can reveal the extent of alveolar destruction and guide clinicians in assessing the severity of the disease. X-rays, while still in use, often yield less detailed information compared to HRCT. However, they can indicate emphysema indirectly through hyper-inflated lungs.
- Common Imaging Techniques:
- HRCT: Effective in visualizing structural damage.
- Chest X-rays: Useful for initial evaluation but has limitations.
Each imaging modality has its unique advantages and signifies the importance of a tailored approach to diagnosis. In many cases, HRCT can spell the difference between a vague clinical picture and a clear diagnosis warranting specific treatment options.
Differential Diagnoses to Consider
Navigating through the diagnostic maze, it’s crucial to keep an eye on potential differential diagnoses that might masquerade as emphysema. Conditions such as chronic bronchitis, asthma, and other restrictive lung diseases could mimic emphysematous symptoms, adding complexity to patient assessment. Unpacking these conditions helps sharpen the focus on the correct diagnosis:
- Conditions to Differentiate:
- Chronic Bronchitis: Often presents with a productive cough, differing from emphysema’s more dyspneic nature.
- Asthma: Characterized by airway hyperreactivity, which can lead to transient symptoms that differ significantly from emphysema.
- Restrictive Lung Disease: Associated with reduced lung volumes, requiring careful assessment to distinguish from the obstructive nature of emphysema.
Ultimately, a thorough understanding of differential diagnoses not only aids in pinpointing emphysema but also enhances the comprehension of a patient's overall respiratory health, leading to better management outcomes.
Treatment Options for Emphysema
Effective management of emphysema is crucial to improving the quality of life for those affected by this disease. Treatment options for emphysema can greatly alleviate symptoms, enhance lung function, and ultimately prolong life. Understanding these options is not only beneficial for patients but also for caregivers, healthcare providers, and public health officials. The primary goal of treatment is to control symptoms while tackling the root causes of the disease, enabling patients to lead a more active life. Exploring various treatment modalities requires insight into their benefits, potential side effects, and the overall lifestyle adjustments they may necessitate.
Pharmacological Interventions
Pharmacological treatments play a pivotal role in managing emphysema. Various medications aim to relax and widen the airways, making it easier for individuals to breathe. Bronchodilators are often prescribed to help open the airways and are essential for reducing breathlessness. There are two primary classifications: short-acting and long-acting bronchodilators. Short-acting ones help relieve symptoms on an as-needed basis, while long-acting options provide extended relief.


- Corticosteroids are another important class of medication. They help reduce inflammation within the lungs and are often used in conjunction with bronchodilators.
- Antibiotics may be prescribed to treat or prevent lung infections, which can complicate emphysema.
Moreover, it’s crucial for patients to understand their medication regimens. Using inhalers and nebulizers correctly can make a significant difference. Tailoring pharmacological treatments to the individual's specific condition is essential for optimal management. For many, a stepwise approach is often needed, adapting as symptoms change over time.
Pulmonary Rehabilitation
Pulmonary rehabilitation is a comprehensive program designed to improve the lung functionality and overall well-being of emphysema patients. This multi-disciplinary approach typically includes physical exercise, education on the disease, nutritional guidance, and psychological support.
- The exercise component is often the cornerstone of pulmonary rehabilitation. It typically includes aerobics, strength training, and breathing techniques aimed at enhancing physical endurance and strength. Patients typically see improvements in their energy levels and overall physical condition.
Engagement in education sessions informs individuals about self-management, thereby empowering them to make informed decisions regarding their health. Coping strategies for dealing with anxiety and depression are also vital, as emotional well-being significantly affects pulmonary function. Importantly, evidence suggests that pulmonary rehabilitation not only helps in managing symptoms but also improves overall quality of life.
Surgical Approaches
In advanced cases where medications and rehabilitation have not provided enough relief, surgical options may be considered. There are two primary surgical techniques for emphysema treatment: lung volume reduction surgery (LVRS) and lung transplantation.
- Lung volume reduction surgery removes damaged portions of the lung, allowing healthier parts to function more efficiently. This surgery is not for everyone and requires careful selection of patients based on their specific health conditions.
- Lung transplantation is often the best hope for particularly severe emphysema cases where other treatments have failed. This procedure offers the potential for a new lease on life but comes with its own set of risks and considerations, including the need for lifelong immunosuppressive therapy to prevent organ rejection.
Choosing the right surgical route involves extensive discussions with healthcare teams, weighing the potential benefits against possible complications.
"Emphysema treatment is not one-size-fits-all; every patient's path to better breathing is unique."
In summary, treatment options for emphysema encompass a range of pharmacological, rehabilitative, and surgical approaches aimed at improving lung function and enhancing quality of life. While each treatment has its pros and cons, tailored strategies can lead to better management of this condition and pave the way for a more rewarding life.
Long-Term Management and Lifestyle Adjustments
Managing emphysema goes beyond treating the immediate symptoms; it encompasses a holistic approach to living with the condition. Long-term management and lifestyle adjustments play a critical role in improving the quality of life for patients. These strategies not only aim to relieve symptoms but also assist in slowing disease progression and enhancing overall wellbeing. While medical treatment is essential, the importance of incorporating lifestyle changes cannot be overstated.
Smoking Cessation Strategies
Quitting smoking is undoubtedly the most impactful change one can make when dealing with emphysema. The damage done by cigarettes is a substantial aggravator of the disease. Evidence shows that stopping smoking can halt further lung deterioration and may improve lung function in some cases.
- To quit smoking, individuals can consider various approaches tailored to their preferences:
- Nicotine Replacement Therapies: Products like patches or gums can help reduce withdrawal symptoms.
- Prescription Medications: Drugs such as varenicline can aid in reducing cravings.
- Support Groups: Joining a community-based group provides emotional support and encouragement.
It's also beneficial to create an environment that helps minimize triggers associated with smoking. Those looking to quit might find it advantageous to avoid situations where smoking is prevalent or seek environments that reinforce their healthy choice.
Nutritional Considerations
Good nutrition is equally paramount in managing emphysema. A balanced diet can strengthen the immune system, improve energy levels, and help patients maintain a healthy weight.
- Nutritional strategies that can have a positive effect include:
- High-Calorie Diets: Some emphysema patients may struggle to maintain weight due to decreased appetite or energy. Foods rich in calories and protein can help.
- Antioxidant-Rich Foods: Consuming fruits and vegetables high in antioxidants can combat oxidative stress and inflammation in the body.
- Hydration: Staying hydrated is crucial; it helps thin mucus in the airways, making it easier to breathe.
Additionally, it can be beneficial to adhere to smaller, more frequent meals rather than large ones, as this can help ease the sensation of breathlessness that often comes with eating.
Exercise and Physical Activity
Engagement in regular physical activity is fundamental for individuals with emphysema. While it sounds counterintuitive to exercise when breathing is labored, tailored exercises can actually enhance lung capacity and endurance.
- Here are several key considerations for incorporating exercise into daily life:
- Pulmonary Rehabilitation: A structured program can educate patients on managing their condition while fostering a workout routine in a supportive environment.
- Breathing Techniques: Techniques such as pursed-lip breathing can improve oxygen flow, making exercise more manageable.
- Low-Impact Activities: Activities like walking, swimming, or cycling can provide cardiovascular benefits without overexerting oneself.
Seek guidance from a healthcare provider to establish a personalized exercise plan. Consistency is key. Even short bouts of activity can equate to significant health benefits over time.
It’s worth emphasizing that clinical support should always be sought before initiating any major lifestyle changes, especially for those with existing health conditions.
In summary, successfully managing emphysema requires a blend of medical treatment, lifestyle adjustments, and a commitment to personal wellbeing. Embracing strategies focusing on smoking cessation, balanced nutrition, and regular exercise can lead to notable improvements in the quality of life for those affected by this chronic condition.
Recent Research Advances
Research into emphysema has taken significant strides in recent years. Innovations in treatment modalities coupled with a deeper understanding of genetic and molecular factors hold promise not only for enhancing patient outcomes but also for potentially altering the course of the disease itself. These advancements illuminate a path forward, encouraging a shift in how we view prevention and management in pulmonary disorders.
Innovations in Treatment Modalities
Recent developments in treatment options for emphysema are indeed noteworthy. One key area of innovation is the use of targeted therapies. Treatments such as bronchodilators and corticosteroids have been improved significantly, now offering better delivery systems and fewer side effects. These newer medications are aimed at relaxing the airways and reducing inflammation more effectively than ever before.
Moreover, researchers are exploring biologics—drugs derived from living organisms—as a novel approach. These therapies, designed to block specific pathways involved in inflammation, target the underlying mechanisms of emphysema rather than merely alleviating symptoms. Clinical trials are currently underway, and early results are showing promising effectiveness in reducing exacerbations and improving lung function.
Advancements in minimally invasive surgical techniques, such as lung volume reduction surgery, have also gained attention. These procedures focus on removing the most damaged areas of the lungs, which can lead to significant health improvements for certain patients.

"Understanding how to manipulate the treatment landscape is vital for patients suffering from emphysema. As research evolves, so must our strategies in the fight against this debilitating disease."
Lastly, the integration of telemedicine and remote monitoring tools allows for closer patient management. This approach not only keeps healthcare providers informed about patient conditions but also facilitates timely interventions, ultimately aiming to mitigate hospital visits and complications.
Genetic and Molecular Research
Another critical front in the fight against emphysema is genetic and molecular research. Studies are increasingly revealing that certain genetic factors can predispose individuals to develop this condition. For instance, alpha-1 antitrypsin deficiency is a notable genetic disorder that heightens the risk of lung damage and emphysema. Identifying these genetic markers plays a pivotal role in early diagnosis and intervention strategies.
At the molecular level, researchers are delving into the cellular mechanisms that lead to alveolar destruction. By understanding the biochemical pathways involved, scientists aim to identify targets for new therapeutic approaches. This research may lead to treatments that effectively halt or even reverse the disease process.
Moreover, understanding the interactions between genetics and environmental factors—like pollution or smoking—can guide public health initiatives. Tailored education and intervention programs might be developed based on genetic risk, helping to ward off the onset of emphysema in at-risk populations.
In summary, the landscape of emphysema research is changing rapidly. Innovations in treatment and insights into genetic factors are setting the stage for more comprehensive prevention and management strategies, ultimately leading to improved quality of life for those affected. The scientific community remains committed to unraveling the complexities of this disease and seeking effective, lasting solutions.
Social and Economic Implications
Understanding the social and economic implications of emphysema sheds light on its broader impact beyond the individual. The burden of this condition is felt not just through personal health struggles but also through financial strain on both healthcare systems and families. When a person suffers from emphysema, it creates ripples that affect employment, community dynamics, and even public health policies.
Healthcare Costs Associated with Emphysema
The financial impact of emphysema on both individuals and health systems is substantial. Healthcare costs can skyrocket due to the chronic nature of this disease. Treatments often include:
- Doctor visits: Constant check-ups and monitoring are essential. The need for specialized pulmonologists can strain budgets.
- Medication: Long-term use of bronchodilators, corticosteroids, and other necessary medications can become a financial burden.
- Emergency care: Exacerbations may lead to hospitalizations, which are expensive and contribute to increased healthcare expenditures.
Overall, it’s estimated that the direct medical costs for managing emphysema and related respiratory conditions can enter the billions annually. Furthermore, indirect costs, such as lost productivity from work absences, also need consideration. Patients often find themselves unable to perform their job functions due to breathlessness or fatigue, which sadly impacts their income and job security, leading to financial distress.
"Every breath can come with a price tag, both literally and figuratively."
Impact on Quality of Life
Quality of life for those diagnosed with emphysema is profoundly affected. One key issue is the loss of independence. Tasks that were once second nature, such as climbing stairs or carrying groceries, become an uphill battle. This shift can lead to feelings of frustration and decreased self-worth.
Moreover, social interactions often take a backseat when out of breath or feeling fatigued. Common activities like:
- Attending family gatherings
- Participating in community events
- Traveling
All become daunting and even impossible. As a result, patients may withdraw from their social circles, leading to feelings of isolation or melancholy.
The mental toll cannot be overstated. Increased anxiety and depression are common among emphysema patients, compounding the physical challenges they face. Through understanding these implications, social support systems and mental health interventions can be initiated to provide necessary help.
Through these lenses, it’s clear that emphysema is not simply a medical issue; it reverberates through family finances, personal relationships, and community health landscapes. Addressing emphysema thus requires an approach that takes into account its broader social and economic ramifications.
Preventive Measures and Public Health Strategies
Preventing emphysema and minimizing its impact on public health deserves significant attention. Strategies that focus on prevention not only safeguard individuals but also reduce the collective burden on healthcare systems. Emphysema often progresses silently, making it vital for public health initiatives to emphasize education, policy, and active community engagement.
Education and Awareness Campaigns
One of the cornerstones of preventing emphysema lies in robust education and awareness campaigns. These initiatives can raise public knowledge about the risks associated with smoking and environmental factors. Effective campaigns highlight how much preventive efforts could change outcomes. Here’s what such programs typically involve:
- Targeted Outreach: Campaigns often tailor messages to specific demographics, ensuring the relevance of the information.
- Community Involvement: Engaging local leaders helps to spread the word more effectively, garnering trust and participation.
- Social Media Engagement: Leveraging platforms like Facebook and Reddit can reach audiences that traditional media may miss.
A successful example comes from the Truth Initiative, which has launched various campaigns aimed at young people, successfully reducing smoking rates and, subsequently, the incidence of emphysema. Such programs underscore the importance of science in health communications and how awareness can lead to behavioral changes.
Policy Implications for Smoking Control
Effective policy measures play a crucial role in combating the incidence of emphysema. Smoking remains the primary risk factor, and strong regulatory frameworks can make a significant impact. Here are some key policy considerations:
- Taxation on Tobacco Products: Increasing taxes on cigarettes and tobacco products has proven effective in reducing consumption, especially among younger populations.
- Smoke-Free Legislation: Establishing smoke-free zones in public spaces reduces secondhand smoke exposure, protecting non-smokers while discouraging smoking behavior.
- Advertising Restrictions: Limiting tobacco advertising, particularly on platforms frequented by youth, can help diminish allure and accessibility.
Policies should be data-driven, reflecting the latest research on the causes and implications of smoking-related diseases. Successful implementation of these policies not only contributes to reducing the incidence of emphysema but also fosters a healthier society, enhancing quality of life for current and future generations.
"An ounce of prevention is worth a pound of cure," rings especially true in the context of emphysema education and smoking control.
Epilogue
The conclusion of this article serves as a vital capstone to our exploration of emphysema, underscoring the multifaceted nature of this serious lung disorder. It's not simply a matter of understanding its clinical aspects; it encompasses a web of social, economic, and personal implications that truly highlight its impact on individuals and communities alike. As we wrap up, it's crucial to reflect on several key elements that have been discussed throughout the article.
First and foremost, the summary of key points around emphysema's pathophysiology, risk factors, and the latest treatment approaches sets a solid foundation for understanding this chronic condition. It’s clear that emphysema is not an isolated problem, but rather one that intertwines with public health issues, economic challenges, and lifestyle choices.
Furthermore, addressing future directions in research is essential. Advances in genetic research, innovative treatment modalities, and improved diagnostic techniques offer hope for better patient outcomes. Such progress signifies not only the evolution of medical science but also the commitment of healthcare professionals and researchers to combat emphysema more effectively.
In essence, the conclusion calls for a proactive stance—cognizance of symptoms, understanding risk factors, and the importance of community awareness and education. Continued research paired with preventive health measures will be pivotal in mitigating the consequences of emphysema. We mustn't underestimate the role of support networks and health policies that align with these aims.
Moreover, by emphasizing the social and economic implications, we bring attention to the broader context in which emphysema exists. It's more than just a medical concern; it shapes the quality of life for many individuals and affects family dynamics and workforce productivity, reverberating through society.
Thus, the importance of understanding emphysema stretches beyond the clinical horizon. It invites individuals, healthcare providers, and policymakers to engage deeply with the topic, fostering a culture of awareness and proactive health management before it affects lives more severely.
"Knowledge is power, and in the context of emphysema, that knowledge can lead to prevention, early detection, and better treatment outcomes."
In summary, this conclusion speaks to the necessity of holistic approaches—balancing medical treatment with emotional and social support—as we move forward in the fight against emphysema.







